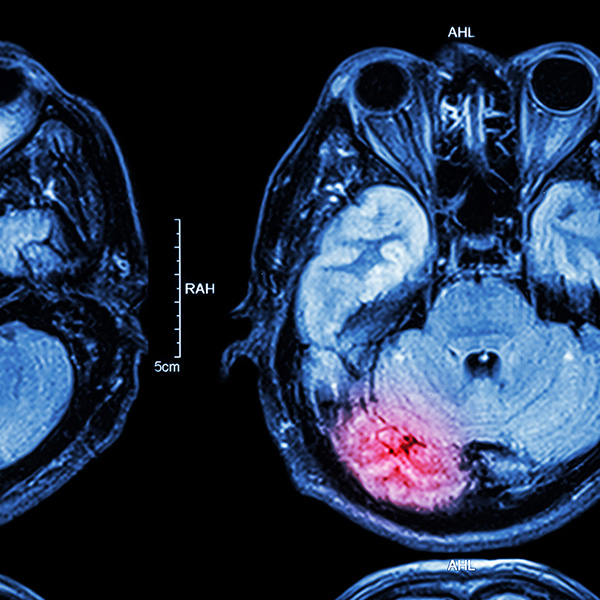
If you or a family/friend have been affected by a head injury, you could be entitled to compensation.
Whilst even relatively minor head injuries can cause far-reaching effects, the most severe brain injuries can be sudden, unexpected and life changing, affecting not only those involved but also those closest to them.
What are the different categories of brain injury?
Traumatic brain injury (TBI)
Often referred to as TBI, traumatic brain injury is an injury to the head or brain caused by some form of external trauma, e.g. the result of a personal assault, a fall or car accident. This trauma causes the brain to move around inside the skull (or damages the skull itself), in turn causing damage to the brain.
Acquired brain injury (ABI)
ABI is the term used to describe any brain injury (inc: traumatic brain injuries) that occur after birth. The most common cause of an ABI is from a build-up of pressure on the brain, e.g. a tumour (unwanted cell growth associated with cancer), or a neurological illness such as a stroke (a blood clot in the brain).
Congenital brain injury (CBI)
Both traumatic and acquired brain injuries refer to an injury that is sustained during or after birth. A congenital brain injury (CBI) is the term used to describe a brain injury that occurs while a baby is still in the womb. It can be caused by disorders, genetic defects, or as a result of something happening to the mother during pregnancy.
8 signs of possible traumatic brain injury
Some signs or symptoms may appear immediately after the traumatic event, while other physical and psychological effects may appear days or weeks later.
A blog by Bradley Wright.
What are the symptoms or examples of different types of brain injury?
Cognitive brain injury (CBI)
A cognitive brain injury is one that impairs a person’s mental abilities. These include problems with memory, attention span, the ability to concentrate, the ability to correctly perceive surroundings, and the speed at which information can be processed.
Symptoms of Cognitive brain injury (CBI)
Memory problems are a very common symptom of brain injury because in order for a brain to process, store and retrieve information, many different areas of the brain must be used at once. If one or more of these areas are damaged, it will affect a person’s memory.
Post-traumatic amnesia (PTA), the medical term for memory loss, is the period of time where the injured person cannot remember what happened either before or after a traumatic brain injury. During this period, the person may find it difficult, or be unable to create new memories.
The severity of the injury will determine the extent of the memory loss, meaning that it can range from the moments just before the accident, to a period of days, months or even years.
PTA is usually temporary, and given time memories can partially or fully return. However it is also possible that these memories will never be recovered, and this again depends on the exact circumstances of the injury.
In cases of permanent memory loss, brain injury rehabilitation efforts are focused on creating coping strategies because as of yet, there is no in-depth scientific understanding of how to reconstitute a person’s memory abilities.
Attention span and concentration are controlled by a part of the brain known as the frontal lobe, so it is very common for someone who has suffered a head injury to have attention difficulties; the inability to multi-task in particular.
In order to regain the ability to concentrate, it is necessary to ‘relearn’ how to do so through rehabilitation and distraction management.
Perceptual difficulties are where the brain is not interpreting the information from our senses correctly. There are a number of wide ranging problems that can result from perceptual difficulties. One example would be when a person may try to pick up a pen but lacks the correct hand-eye coordination to do so. Despite being able to see the pen, they cannot accurately determine its position relative to their hand because of an issue with judging distances and spatial relationships. Another example would be the inability to recognise a common object when it is viewed from a non-standard angle.
The brain may have reduced ability to process larger amounts of information in small spaces of time, usually due to changes in neural pathways. A useful analogy for this would be if the road system covering your journey to work was completely changed, then it would take you much longer to find your way to work than before.
Slower information processing will result in issues such as requiring people to speak slower, the need to be given instructions several times before they are understood, and difficulties in replying to questions in a ‘normal’ amount of time. These symptoms can be described as the person being constantly in a state of ‘information overload’.
Physical brain injury
As well as housing our thoughts, memories and personality, the brain also coordinates the subconscious physical processes that are essential to a healthy life such as breathing, hormonal balance, blood pressure regulation, the digestive system and body temperature regulation. Without these functions, our bodies would not operate correctly and cause an exceptional amount of day-to-day living difficulties.
A severe brain injury can cause irreparable damage to the brain’s ability to control these regular functions, so rehabilitative efforts shift from fixing the problem to learning how to cope with them. In severe cases, full-time carers may be required.
Physical brain injury examples
- Movement, balance, and coordination problems
- Fatigue
- Chronic pain
- Spasticity
- Incontinence
- Epilepsy
- Loss of sensation
- Headaches
- Dysarthria
- Dyspraxia
- Hormonal imbalances
Behavioural/emotional brain injury
A brain injury can sometimes ‘rewire’ a person’s personality, causing their behaviour and emotional reactions to change. Exactly what is changed will depend upon which parts of a person’s brain are injured e.g. the frontal lobe controls our personality and our impulsivity.
If this area of the brain becomes damaged after injury, it is possible that the person has reduced self-control or restraint and may not be able to moderate their emotions, resulting in irrational behaviour. The person may also go to the other extreme, and have what seems to be an emotionless personality. This is known as “flat affect”. These types of symptoms are perhaps less obviously noticeable than physical problems, but also have a large impact.
It is often the case that the injured person does not realise that they are now acting differently compared to how they were before.
• Mood swings
• Lack of judgement, awareness and disinhibition
• Agitation
• Apathy
• Depression
• Self-centredness
• Obsession
• Anxiety
• Inflexibility / stubbornness
• Sexual problems
Mood Swings
A brain injury can sometimes change a way that a person feels or expresses their emotions. Damage to the frontal lobes may mean that they lose the ability to regulate their emotions, and experience random mood swings that are unrelated to how they are actually feeling.
Unpredictable outbreaks of laughter or crying are common and they may feel like they are on an ‘emotional roller-coaster’. They may have a reduced tolerance for stress and frustration, so even something as minor as having the television volume too loud or losing a set of keys can lead to an extreme verbal or physical outburst.
e.g: seemingly random changes from one emotion to another
Lack of judgement, awareness and dis-inhibition
The ability to evaluate and adjust our personal behaviour to the circumstances around us is a complex skill, largely controlled by the brain’s frontal lobes. Damage to this area can affect self-awareness, insight into the consequences of one’s actions, and ability to show empathy or sensitivity. Those injured may also be unable to distinguish when they are being impolite or breaching social etiquette.
e.g: touching someone inappropriately, speaking your mind regardless of the circumstances, recklessness.
Agitation
It is not uncommon for a recently injured person to be uncooperative due to disorientation, confusion and anxiety. They may do things like pull out their IV tubes or experience restlessness because the behaviour acts as a coping mechanism to relieve the stress of the situation. An unusual level of agitation is most often a temporary symptom, going away with time as the person becomes less confused by their situation.
e.g: restlessness, fidgeting, pacing.
Apathy
Damage to the frontal lobe can also cause a lack of motivation or spontaneity. This is because the person has reduced levels of emotion and forward planning, which makes activities appear extremely overwhelming.
e.g: staying in bed all day, a lack of interest in previous hobbies.
Depression
Once the rehabilitation process starts, it is very common for the person to experience depression. This is especially the case towards the later stages of rehabilitation, as they realise the full extent of the problems caused by their injury and any permanent damage that they will have to cope with.
It is worthwhile to note that depression is an important stage of mental recovery, because it means they are aware of the reality of their situation. Only then can the person begin to accept the situation and move forward.
e.g: wishing they had not survived the accident, believing life will never be good again.
Anxiety
It is normal for an injured person to suffer from anxiety, due to the loss of confidence they experience with situations and tasks that used to be commonplace but are now difficult, e.g. if the person has writing difficulties, they may be worried about signing documents.
It is important that these difficult situations are faced head on, with an attitude of independence in mind, because if these fears are left to fester then the more likely they are to become a long-term problem.
e.g: panic attacks, paranoia, poor quality sleep.
Inflexibility and obsessionality
The frontal lobe is where our ability to reason and make sense of things originates. If damaged, the person may be unable to do things differently, and stubbornly stick to a routine or habit. This is because they have lost the ability to consider alternatives on their relative merit, and make a decision based on that analysis. Anxiety will make this worse because the injured person may think that sticking to a routine will make them feel better.
e.g: strange patterns of behaviour, unreasonable stubbornness, over-attachment to belongings.
Sexual problems
A person’s sex drive can either increase or decrease. There are a great many physiological and psychological reasons for this, most of which are due to the hypothalamus (an important structure in the brain which controls hormone levels) being over or under-active.
e.g: increase or decrease in sex drive, misinterpretation of sexual advances
It doesn’t stop there…
Edwards Duthie Shamash provide you with help and advice along the way. We also refer you for additional support so that you are able to adjust to new circumstances following the Head or Brain injury. We can advise about care, rehabilitation and life skills; providing you with any essential custom aids and appliances.
Whatever is needed for you and your case, we help to put it in place.
Personal Injury FAQs
Each personal injury claim is different and the amount of recoverable compensation will depend upon the severity of your injuries, whether you are partly responsible for the accident, how much you have lost in earnings and whether you have made a recovery or whether you require further treatment.
Please click our personal injury compensation calculator to obtain further information about personal injury damages.
If your claim is successful you will receive one total sum that is arrived at by combining two heads of damage, namely general damages and special damages. General damages is an award of money that is given to you purely in relation to the injury you have suffered and takes into account pain and suffering, loss of amenity, severity of injury and whether any ongoing treatment and care is required.
Special damages are all those losses and expenses you have incurred as a direct result of the accident including loss of earnings, loss of pension, medical treatment, ongoing care and rehabilitation, travel expenses and modifications to your home.
You usually have three years in which to make a personal injury claim. This is usually three years from the date of your accident or three years from the diagnosis of a workplace illness. On occasions, the three year period will also run from the date on which you learned that your injury or illness was caused by somebody else.
There are some exceptions to the above period, and therefore it is best to get in touch with us as soon as possible. This will give our personal injury solicitors every opportunity of obtaining the relevant evidence that they need to successfully make your claim. We will be able to advise you of the exact legal deadline and will still be able to help you if the deadline is approaching.
You can claim damages to reflect the injury that you have sustained. This is known as general damages and takes into account pain, suffering, loss of amenity, how seriously injured you are and whether you have made a full recovery or not.
Any compensation claim would also include any financial losses you have suffered including loss of earnings, loss of pension, costs of medical treatment and travel expenses and costs of any rehabilitation and care, if needed.
Serious injuries are those which will have a long-term effect and are life-changing. Compensation for these injuries must take into account:
• Rehabilitation needs
• Long-term care and support
• Loss of earnings and pensions if you are no longer able to work or cannot perform the same job
• Moving to a new home or making adaptations to your existing home
Serious injury claims usually take a few years to bring to a conclusion. However, it is possible for us to obtain interim compensation payments before the conclusion of your claim, to help pay for any treatment you require. These payments are available if the responsible party admits fault for your injury. The final settlement will depend upon a number of factors including whether you have made a full recovery or not. Our specialist lawyers will make sure that your compensation is calculated to take into account all relevant factors.
The value of your claim depends on a number of factors but generally there are two categories:
1. Compensation for your Personal Injury
2. Compensation for your financial losses
We will help you understand the likely level of compensation you could receive providing:
• A full assessment of the extent of your injuries
• The type of injury sustained
• Your symptoms and their duration
• Advice on what can be claimed for
There are many ways of funding your personal injury case and we will advise you of the best option. We offer a genuine “NO WIN NO FEE” agreement and if you choose this arrangement you should have nothing to pay if your claim is unsuccessful.
We will also consider obtaining an insurance policy to be in place to pay your opponents costs should you be required to pay anything. If there is ever a situation whereby you may be required to pay something you will be advised of this possibility well in advance so that you can avoid it arising should you wish to do so.

Edwards Duthie Shamash will help you with your Personal Injury claim efficiently and as quickly as possible
Support for anyone adjusting to life after sustaining a Brain Injury is imperative and that’s why we’re here to help you. We specialise in high-level injury cases and are proud of our ongoing achievements allowing us to secure multi-million pound compensation awards for our clients providing life-long financial stability.
We have provided specialist legal assistance for over 120 years to individuals, families and businesses.
We offer a free consultation with legal advice and will be able to handle your claim on a No Win No Fee basis. We will endeavour to remove any added stress by dealing with your claim in a diligent and compassionate manner.
We’re experienced and compassionate.
Our solicitors have extensive experience in handling claims and have recovered compensation for thousands of clients. We work on a No Win No Fee basis and do our utmost to recover the compensation that you deserve in a friendly and diligent manner.